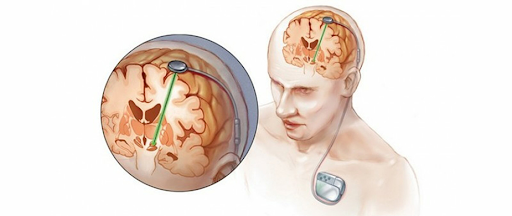
Deep Brain Stimulation is a treatment used for certain neurological conditions that affect movement and daily life, including Parkinson’s disease, dystonia, and essential tremor. The procedure involves placing electrodes in specific areas of the brain to help regulate abnormal nerve signals and improve symptom control. Before surgery, patients undergo a detailed medical evaluation to assess their condition, treatment response, and overall health. This process helps determine whether the procedure is suitable and prepares patients and caregivers for treatment and recovery.
Understanding the Purpose of Pre-Surgery Evaluation
The evaluation before surgery helps doctors determine whether Deep Brain Stimulation is suitable for the patient’s condition and medical history. Specialists carefully review symptoms, treatment response, and overall health to understand whether the procedure may improve symptom management and daily functioning. The assessment also helps identify medical concerns that could affect surgery or recovery. In many cases, neurologists, neurosurgeons, psychologists, and rehabilitation specialists work together during the evaluation process to support safer treatment planning and informed decision-making for patients and families.
Medical History and Symptom Review
The first stage of evaluation usually focuses on understanding the patient’s medical background, symptom history, and current treatment plan. Doctors review how symptoms have progressed over time and whether daily activities have become difficult due to movement-related challenges.
- Duration of Symptoms: Doctors assess how long the patient has experienced tremors, stiffness, balance issues, or slow movement.
- Medication Response: Current and previous medicines are reviewed to understand symptom control and treatment effectiveness.
- Daily Activities: Specialists may ask how symptoms affect walking, speaking, eating, or routine activities.
- Existing Medical Conditions: Conditions such as diabetes or heart disease are reviewed before surgery planning.
This information helps specialists understand whether the patient may benefit from DBS surgery and whether further assessments are needed before surgery planning begins.
Neurological Examination
A neurological examination helps doctors assess movement-related symptoms before planning surgery. Specialists evaluate coordination, posture, walking pattern, muscle stiffness, and tremor severity to understand how the condition affects daily functioning. For people with Parkinson’s disease, assessments may be performed when medication is working and again when symptoms return. Comparing these observations helps doctors determine whether stimulation therapy may improve movement control and whether the patient is likely to benefit from surgical treatment.
Brain Imaging Tests
Brain imaging tests help specialists study the brain’s structure before surgery and support accurate treatment planning. MRI or CT scans are commonly recommended to identify the target areas for electrode placement during the procedure.
- MRI Scans: MRI helps doctors examine brain structure and identify treatment targets before surgery.
- CT Scans: CT imaging may support surgical planning and evaluation in certain cases.
- Assessment of Brain Health: Imaging helps identify abnormalities that may increase surgical risk.
- Treatment Planning: Scans support accurate electrode placement during the procedure.
These imaging results are carefully reviewed by the surgical team before deciding whether the patient is medically suitable for Deep Brain Stimulation treatment.
Cognitive and Psychological Assessment
Cognitive and psychological assessment is an important part of pre-surgery evaluation. Some neurological conditions may affect memory, focus, mood, and decision-making, which can influence recovery and long-term symptom management. Patients may undergo tests for memory, language, attention, and thinking ability. Psychological evaluation also helps identify anxiety, stress, or depression so doctors can provide balanced support during recovery.
Physical Health Assessment
General physical fitness is carefully assessed before surgery to ensure the patient can safely undergo the procedure and recover. Doctors usually recommend routine health tests to identify medical concerns that may affect surgical safety, postoperative recovery, and monitoring.
- Blood Tests: Routine tests help assess overall health before surgery planning.
- Heart Evaluation: Doctors may recommend heart-related tests to assess cardiovascular fitness.
- Anaesthesia Assessment: Anaesthesia specialists may discuss surgical precautions and safety measures.
- Infection Screening: Existing infections or health concerns may require treatment before surgery.
These evaluations help reduce surgical risks and allow doctors to prepare an appropriate treatment plan based on the patient’s overall health condition.
Discussion About Treatment Expectations
Before surgery, doctors discuss the expected benefits and limitations of treatment with patients and caregivers. Deep Brain Stimulation may improve movement symptoms and reduce certain medication-related complications, although it may not completely remove all symptoms experienced by the patient. Patients are also informed about follow-up appointments, device programming sessions, and ongoing postoperative monitoring. Recovery and symptom improvement may occur gradually, so clear communication helps patients maintain realistic expectations and make informed, confident treatment decisions.
Conclusion
The evaluation process before DBS surgery helps doctors determine whether the procedure is suitable, safe, and likely to benefit the patient. It includes medical review, neurological examination, brain imaging, cognitive assessment, and physical health checks. A careful and compassionate assessment allows specialists to plan treatment according to the patient’s condition while supporting safety, comfort, and long-term care needs.